Donor Care Units in Upper Midwest
Donor care units (DCU) are dedicated clinical facilities focused on providing optimal and efficient care of organ donors prior to organ donation as well as the most advanced organ recovery techniques, which can improve the opportunities for organs to be successfully transplanted into waiting recipients.
Please don’t hesitate to call LifeSource at 1-800-247-4273 for real-time assistance. Your responsibility is to educate yourself on the policies and procedures at your hospital, specifically.
LifeSource, Mayo Clinic and M Health Fairview to Establish “Donor Care Units”
In July 2023, LifeSource, Mayo Clinic and M Health Fairview announced a collaboration to create a system of “Donor Care Units” to increase the number of lives saved through organ donation in the upper Midwest.

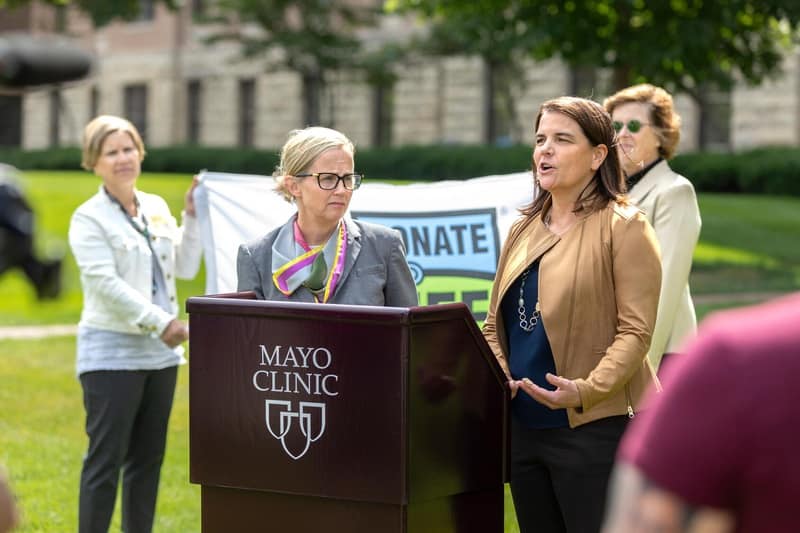
How DCUs Work:
- Individuals who have authorized organ donation (by registering on their driver’s license or the online donor registry; or their family authorizes on their behalf at the time of death) and meet donation criteria (brain death or non-survivable injury) are transferred from a hospital intensive care unit (ICU) to a dedicated donor care unit at Mayo Clinic or M Health Fairview University of Minnesota Medical Center.
- Hospitals will still conduct typical ceremonies to honor donors – like an honor walk or flag raising – as part of the donor transfer to a DCU.
- Donor care, organ health management, matching/allocation and recovery will occur at the DCU.
Benefits of DCUs include:
- Increased capacity at donor hospital facilities: Transferring to a DCU improves access to critical care beds and operating room facilities at the referring hospital. Donors will still be attributed to the hospital where the donor referral was made, not by where the recovery occurs.
- More organs recovered; more lives saved: DCUs will have dedicated donor management staff and facilities including sophisticated imaging and diagnostic equipment (such as X-ray, bronchoscopy, CT scanner, cardiac catheterization labs and point-of-care laboratory services). Devices – like organ care systems – may also be housed onsite.
- Family support: DCUs also allow for a faster organ recovery, which benefits donor families: the time required to complete the process – including securing the OR space and surgical team – is often why families decline donation.
Donor Care Units Explained
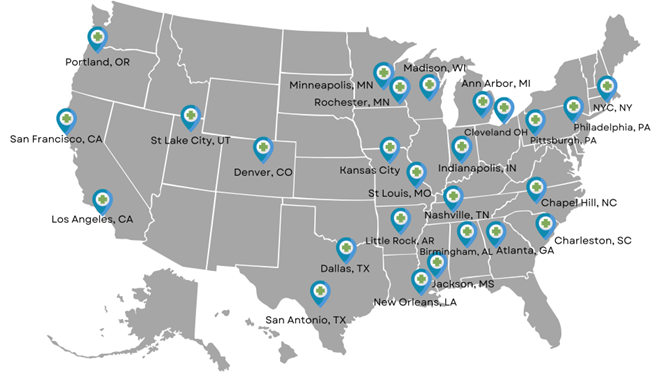
In the United States, 24 of the 55 Organ Procurement Organizations (OPOs) have active DCUs, as of December 2022. A majority of the remaining OPOs report current or pending development of Donor Care Units.
Hospitals in this service area provide state-of-the-art patient care and have developed excellent donation programs. This change will only build upon the commitment to organ, eye and tissue donation that hospitals have demonstrated, and the donor and family care you’ve provided.
DCUs have become the standard for donor care and management, based on research showing dramatic improvement in organ recipient outcomes. This research shows that these outcomes are not due to failures of clinical management, but instead relate to intensive, dedicated use of time, staff and resources that is not possible or feasible in every hospital. For example, an RT performing lung recruitment hourly may be able to convert non-transplantable lungs into life-saving gifts.
Outcomes of donor care units across the country have seen donation most optimized at transplant hospitals that have both abdominal and cardiothoracic transplant programs.
“DCUs relieve the strain on hospital resources required for the process of donor evaluation, management, and organ recovery. Centralizing OPO dedicated resources to provide these services in a space that doesn’t compete for hospital resources, allows the process to move quicker, which means life-saving organs can be on their way to a transplant center sooner and ultimately, positively impact recipient outcomes.”
Source: Maximizing the gift with a donor care unit: The OPO-based approach. The Organ Donation and Transplantation Alliance. (n.d.).
Life-saving donation occurs because hospital care teams believe in it, provide exceptional care, support donation opportunities, and notify LifeSource of potential donors. These elements open the door for generous individuals and families to save lives while creating a legacy of generosity, hope and healing.
Hospital care teams share that it is an honor to care for patients and their families at pivotal moments in their lives. That will not change.
Current practices to honor the donor, family, and legacy will continue. These may include developing the Moment of Silence to be read during OR, flag raisings, honor walks to be held during the transition to helipad or ambulance bay.
Donors initiated at each hospital will be attributed to hospital donation program outcomes, and initiating hospital location will be used for allocation location.
Local Experience
Regions nurses have been participating in the transfer process since September 2022. They have expressed positive experience with this process for their donor patients and families. They have emphasized the continued strength of their hospital donation program, highlighting meaningful program elements that did NOT change:
- Exceptional patient care is provided at our hospital.
- Our LifeSource referral process did not change.
- Brain death testing is done by our providers.
- We connect families with LifeSource for donation conversations.
- We still have flag raisings for our families.
- Honor walks are still incredibly meaningful and are more predictable. (They happen on the way to the ambulance bay for donor transfer instead of to the OR.)
- We still feel connected to the donor and donor family.
- Annual Gift of Life Memorial Ceremony.
- We still receive Donor Outcome Emails sharing what gifts were recovered.
Transfers to M Health Fairview in Minneapolis: All hospitals within 7 county Twin Cities metro area and St Cloud.
Transfers to Mayo Clinic in Rochester: Hospitals outside Twin Cities metro, and all of North Dakota and South Dakota hospitals.
LifeSource will coordinate admission to the DCU hospital. These DCUs have committed to accepting donor patients. A care team to care team connect will be arranged by LifeSource and may include APP connections, RN to RN report, and, if necessary, MD to MD connect.
Donor critical care transport will be arranged and managed by donor care units. For Mayo Clinic, transport will primarily be done by Mayo One Flight. For the University of Minnesota, transport will primarily be done by Fairview EMS ground services. LifeSource will partner with your hospital to ensure your local EMS teams are aware this is happening.
Some of the stability criteria* considered for transport to DCU:
- Chest x-ray prior to transport with documentation that ETT position is adequate (2-6 cm above carina)
- Cervical spine stabilization if traumatically injured
- Oxygenation and ventilation – optimization of blood gas values
- PaO2/FiO2 ratio ≥ 150 on FiO2 ≤ 70% and PEEP ≤ 12
- PaCO2 ≤ 60 with Tidal volume ≤ 8 mL/kg and RR ≤ 30
- pH between 7.3-7.5
- If pneumothorax present, chest tube should be inserted and placed on 20 cm H2O suction throughout transport process
- At least 2 vascular access points. For example, large bore Peripheral IVs and/or central access
- Inopressor requirements
- ≤ 3 total inopressors to maintain MAP > 65
- Doses:
- Epinephrine and/or norepinephrine ≤ 0.2 mcg/kg/min
- Vasopressin ≤ 0.04 U/min
- Phenylephrine ≤ 2 mcg/kg/min
- Volume resuscitation
- Base excess ≥ -10
- Bicarbinate level ≥ 14
- Any external or internal hemorrhage should be adequately controlled
- If Extra Ventricular Drain present, will need documentation of hernation. If this is not possible, it is also reasonable to remove this device.
*Thanks to Dr. Randy Mielke, Mayo Clinic, for contributing these criteria.
The overwhelming national experience with DCUs has been that families of potential donors accept transfer as part of standard donation process and report positive experiences with donation overall.
In the rare event that a family objects to their loved one’s transfer or a patient is too unstable to transfer to a DCU, LifeSource will partner with the hospital on accommodating a local recovery.
Nationally, most families have said goodbye to their loved one at the hospital prior to their loved one’s transfer to the Donor Care Unit. Additionally, families have shared a sense of relief when they are provided the guidance that they can say goodbyes and return to their homes. Therefore, travel will not be offered to families as standard.
While the exception, for those families who request to travel with their loved one, each DCU hospital has committed to providing resources and support for families. These resources include assistance with travel and accommodation.
LifeSource will continue to reimburse the initiating hospital charges that are related to donation. LifeSource’s finance team works closely with hospital Patient Billing contact to review charges. All bills will be reviewed and paid according to CMS’s guidelines on hospital costs for donation, which are intended to cover costs and avoid undue burden on hospitals. Hospitals will not lose reimbursement opportunity by transferring donors.
LifeSource Finance Team is available to discuss additional specific questions: ap@life-source.org.
LifeSource arranges transport to the funeral home that the family has selected. All donation-related costs are covered by LifeSource. No donation-related expenses are covered by families.
Transfers to Mayo Clinic Donor Care Unit: Presentation & Discussion with Hospitals
*Note: This presentation focused on education surrounding transfers to Mayo Clinic.
Additional Resources
For more information regarding the Donor Care Units, check out these resources.
 Skip to main content
Skip to main content
